Tackling Childhood Obesity in Mississippi – A Systems Thinking Approach
Childhood obesity is a critical public health issue that has far-reaching implications for individuals, communities, and healthcare systems. In Mississippi, where childhood obesity rates are alarmingly high, addressing this complex problem requires a multifaceted, systems-thinking approach that involves multiple sectors and levels of intervention. This discussion will explore the use of systems thinking tools, specifically process mapping and causal loop diagrams, to depict how a community and a public health system might tackle childhood obesity in Mississippi. In addition, it will emphasize the multilevel and multisectoral strategies that can be implemented, considering different age groups.
Process Mapping: Community-Level Strategies
Early Childhood (Ages 0-5)
In the early childhood stage, community-level strategies are essential to prevent childhood obesity from developing. Process mapping reveals several key components: Maternal and Child Health Services, Early Childhood Education, Community Engagement, and Access to Safe Playgrounds.
Maternal and Child Health Services
Firstly, start by providing comprehensive maternal and child health services, including prenatal and postnatal care, to support healthy pregnancies and early child development. Also, ensure access to resources like WIC (Women, Infants, and Children) for nutritional support.
Early Childhood Education
Next, develop high-quality early childhood education programs that emphasize nutrition and physical activity. This includes integrating nutrition education into preschool curricula and ensuring children have access to balanced meals.
Community Engagement
Community engagement includes engaging parents, caregivers, and local organizations in promoting healthy behaviors (Economos et al., 2023; Kasman et al., 2019). It also includes establishing community gardens to encourage the consumption of fresh produce and organizing events that emphasize physical activity.
Access to Safe Playgrounds
Further, provide safe and accessible playgrounds to promote physical activity. Additionally, ensure neighborhoods have sidewalks and safe streets to encourage walking and biking.
School-Age Children (Ages 6-18)
The key components for this age group include School-Based Interventions, Family Involvement, Local Policies, and Community Partnerships.
School-Based Interventions
In this step, one should implement process mapping at the school level to improve students’ nutritional intake and physical activity (Bejster et al., 2022; Lambrinou et al., 2020). This may include healthier school meal options, nutrition education, and mandatory physical education classes.
Family Involvement
One can promote family involvement by educating parents about nutrition and exercise. Family involvement can also be promoted by encouraging parents to pack healthy lunches for their children and support after-school physical activities.
Local Policies
This involves advocating for local policies that restrict the sale of unhealthy foods and beverages near schools and establishing safe walking and biking routes to schools.
Community Partnerships
Lastly, community partnerships can be formed through collaboration with local businesses, community organizations, and healthcare providers to create a supportive environment for children to make healthier choices.
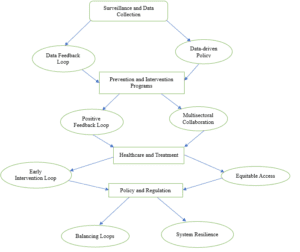
Causal Loop Diagram: Public Health System-Level Strategies
Surveillance and Data Collection
Data Feedback Loop
To begin with, the public health system should continuously collect and analyze data on childhood obesity rates, risk factors, and intervention outcomes. Feedback from these data should drive policy and program adjustments.
Data-Driven Policy
Next, policymakers should use the data to inform policy decisions, targeting areas with the highest childhood obesity rates and directing resources accordingly.
Prevention and Intervention Programs
Positive Feedback Loop
This step involves implementing evidence-based prevention and intervention programs that target childhood obesity (Bejster et al., 2022; Economos et al., 2023; Kasman et al., 2019; Lambrinou et al., 2020). As these programs succeed, they contribute to lower obesity rates, creating a reinforcing feedback loop.
Multisectoral Collaboration
Further, multisectoral collaboration, for instance, the collaboration between the education, transportation, and agriculture sectors, can create a holistic approach to obesity prevention. For example, the agriculture sector can support local food production, making healthy options more accessible.
Healthcare and Treatment
Early Intervention Loop
Here, it should be ensured that healthcare providers are trained to identify and address childhood obesity early (Bejster et al., 2022; Economos et al., 2023; Kasman et al., 2019). Subsequently, this leads to earlier interventions, reducing the risk of severe health consequences.
Equitable Access
For equitable access, healthcare disparities should be addressed by improving access to obesity prevention and treatment resources, especially for underserved populations.
Policy and Regulation
Balancing Loops
This would involve developing and implementing policies that regulate food marketing to children, limiting sugar and unhealthy fat content in food products, and creating urban planning that encourages physical activity (Economos et al., 2023; Kasman et al., 2019; Lambrinou et al., 2020). Notably, these policies counteract the obesogenic environment.
System Resilience
Regarding system resilience, it should be ensured that policies remain adaptable to changing circumstances, such as emerging dietary trends or new research on obesity prevention.
Conclusion
In summary, tackling childhood obesity in Mississippi is a multifaceted challenge that demands a systems thinking approach at both community and public health system levels. Process mapping and causal loop diagrams help visualize the complex interplay of factors and strategies involved. It is crucial to recognize that the fight against childhood obesity is not confined to a single sector or age group. Instead, it requires a comprehensive, multilevel, and multisectoral effort that engages families, schools, healthcare providers, policymakers, and communities. By using systems thinking tools, Mississippi can take significant steps toward a healthier future for its children, fostering a culture of well-being and making strides in reducing childhood obesity rates.
References
Bejster, M., Cygan, H., Stock, J., & Ashworth, J. (2022). A school wellness partnership to address childhood obesity. Progress in Community Health Partnerships: Research, Education, and Action, 16(1), 85–91. https://doi.org/10.1353/cpr.2022.0008
Economos, C. D., Calancie, L., Korn, A. R., Allender, S., Appel, J. M., Bakun, P., Hennessy, E., Hovmand, P. S., Kasman, M., Nichols, M., Pachucki, M. C., Swinburn, B. A., Tovar, A., & Hammond, R. A. (2023). Community coalition efforts to prevent childhood obesity: two-year results of the Shape Up Under 5 study. BMC Public Health, 23(1). https://doi.org/10.1186/s12889-023-15288-5
Kasman, M., Hammond, R. A., Heuberger, B., Mack‐Crane, A., Purcell, R., Economos, C., Swinburn, B., Allender, S., & Nichols, M. (2019). Activating a community: An agent‐based model of romp & chomp, a whole‐of‐community childhood obesity intervention. Obesity. https://doi.org/10.1002/oby.22553
Lambrinou, C.-P., Androutsos, O., Karaglani, E., Cardon, G., Huys, N., Wikström, K., Kivelä, J., Ko, W., Karuranga, E., Tsochev, K., Iotova, V., Dimova, R., De Miguel-Etayo, P., M. González-Gil, E., Tamás, H., Jancsó, Z., Liatis, S., Makrilakis, K., & Manios, Y. (2020). Effective strategies for childhood obesity prevention via school-based, family-involved interventions: a critical review for the development of the Feel4Diabetes-study school-based component. BMC Endocrine Disorders, 20(52), 1–20. https://doi.org/10.1186/s12902-020-0526-5
ORDER A PLAGIARISM-FREE PAPER HERE
We’ll write everything from scratch
Question

Tackling Childhood Obesity in Mississippi
Using systems thinking tools, such as process mapping, stock and flow diagrams, or causal loop diagrams, depict how a community and a public health system might tackle obesity in Mississippi. For example, you will create two illustrations using the systems thinking tool described above. Your depictions should emphasize the multilevel and multisectoral strategies that each could possibly take. Students may tackle any age group because strategies would differ depending on age. This is a 3-4 page paper using the APA (7th edition) writing style. Students will also provide a narrative that summarizes their system thinking illustration. A final paragraph should include policy recommendations and possible synergies to reduce costs.