Patient Medication Guide
Medication Study Guide: Chlorpromazine
Brand and Generic Names
Chlorpromazine is a conventional antipsychotic drug with the brand name Thorazine, and it belongs to the family of phenothiazines. The drug is among the first-generation antipsychotic medications, and it has been widely used for a long time after its introduction to the market. This medication has immensely eased the treatment of psychiatric disorders by handling psychotic features.
FDA Indication Uses
Chlorpromazine is an antipsychotic drug that is majorly administered for the control of psychotic disorders like schizophrenia and bipolar disorders. It is useful in the management of these symptoms to alleviate hallucination, delusion, and agitation in such disorders. Further, it is used where there is nausea and vomiting, chronic hiccups, acute intermittent porphyria, and severe behavioural disorders in children. This drug has many indications and thus can be administered in psychiatric practice as well as general medical practice.
Supporting, Valid, and Reliable Research for Non-FDA Uses
Research done by Stip et al., (2020) has shown that chlorpromazine can be effective in managing severe agitation in patients with dementia and treating intractable migraine headaches. Studies indicate that chlorpromazine, despite not being FDA-approved for these indications, can provide significant relief. Its use in these areas is based on valid and reliable clinical evidence, highlighting its potential beyond the primary FDA-approved uses (Nucifora et al., 2019).
Drug Classification
Chlorpromazine belongs to the class of first-generation antipsychotics, also known as typical antipsychotics. These medications are known for their ability to block dopamine receptors in the brain, which helps in reducing psychotic symptoms. The classification of chlorpromazine as a typical antipsychotic is due to its pharmacological properties and mechanism of action, which distinguish it from second-generation or atypical antipsychotics.
Mechanism of Action
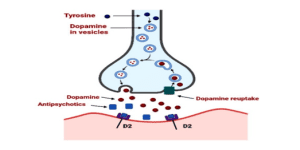
Chlorpromazine, on its own, is an antagonist of dopamine receptors, especially the D2 receptors in the brain. This blockade aids in the diminution of positive symptoms of psychosis, such as hallucinations and paranoid delusions. Chlorpromazine is also an anticholinergic and antihistaminic agent, and it possesses alpha-adrenergic blocking properties in addition to its antipsychotic action. These additional actions are responsible for its therapeutic effects and side effect liability.
Pharmacokinetics
Chlorpromazine is known to be a drug that can be taken orally with efficiency, though its bioavailability is reduced due to first-pass metabolism in the liver. It is present in different tissues and penetrates through the blood-brain barrier to affect the CNS. (Mann & Marwaha, 2023). The drug is metabolized in the liver primarily by CYP2D6 and CYP1A2 enzymes and is excreted mainly through urine, with some excretion in feces.
Pharmacodynamics
The pharmacodynamics of chlorpromazine involve its action on dopamine receptors, leading to the alleviation of psychotic symptoms. By antagonizing D2 receptors, chlorpromazine reduces the overactivity of dopamine in certain brain regions, which is believed to be a key factor in the manifestation of psychosis. Its additional effects on other neurotransmitter systems contribute to both its therapeutic benefits and potential side effects.
Dosing, Administration Route, and Considerations for Dosing Alterations
For adult patients with schizophrenia, chlorpromazine is typically administered orally in doses ranging from 10-25 mg three times daily, with gradual increases to a maintenance dose of 200-800 mg daily. For nausea and vomiting, the usual dose is 10-25 mg every 4-6 hours as needed (Gammon et al., 2021). Chlorpromazine can be administered orally, intramuscularly, or intravenously. Dosage adjustments are necessary for elderly patients, those with liver impairment, and during pregnancy to minimize adverse effects and ensure safety.
Specialty Populations Considerations
In children, chlorpromazine should be used with caution, and doses must be carefully calculated based on weight. For elderly patients, lower initial doses with gradual increments are recommended due to increased sensitivity to side effects. During pregnancy, chlorpromazine should only be used if the potential benefit justifies the potential risk to the fetus. For patients exhibiting suicidal behavior, close monitoring is required due to the increased risk of sedation and possible worsening of depression.
Half-Life
The half-life of a medication is the time required for its concentration in the plasma to reduce by half. This parameter is important because it helps one ascertain the dosing frequency and how long the drug’s effect will take. The elimination half-life of chlorpromazine is around 30 hours. However, the knowledge of the half-life is vital for clinicians to be able to set the right dosing intervals and to determine the time of action of the drug’s therapeutic as well as toxic effects.
Side Effects/Adverse Reactions Potential
The side effects that are related to chlorpromazine include sedation, postural hypotension, anticholinergic effects, blurred vision, weight gain, and gastrointestinal dysfunction. Some of the serious side effects are neuroleptic malignant syndrome, tardive dyskinesia, and extrapyramidal symptoms. Such possible side impacts should be adequately supervised, and patients should be well-advised if they appear.
Clinical Concerns with EPS and Tardive Dyskinesia
Chlorpromazine causes extrapyramidal symptoms (EPS) and tardive dyskinesia in clinical practice. It consists of symptoms like tremors, rigidity, and bradykinesia, while TD is a syndrome manifested in irregular, involuntary movements and can be late-emerging and permanent in nature. Assessment tools such as the Abnormal Involuntary Movement Scale (AIMS) are useful, as they may reveal the presence of these disorders and help to make necessary alterations in treatment plans and approaches.
Contraindications for Use Including Significant Drug-to-Drug Interactions
Chlorpromazine is contraindicated in patients having known sensitivity to this drug, in comatose patients, or in patients with significant CNS depression. It should not be given with other agents that cause central nervous system depression or anticholinergic products since this will exaggerate its effect (Harbell et al., 2021). Besides, using chlorpromazine may interfere with dopamine agonists as they will lose their effectiveness and should, therefore, be used carefully together. These contraindications and interactions must be thoroughly understood when utilizing chlorpromazine.
Overdose Considerations
In the event of an overdose, symptoms may include severe CNS depression, hypotension, and extrapyramidal symptoms. Intervention entails supportive measures, activated charcoal within an hour of ingestion, and responding to clinical signs. The management of overdose involves early identification and proper intervention to mitigate the effects and risks to the patient’s life.
Diagnostics and Labs Monitoring Comorbidities Considerations
Patients on chlorpromazine should be monitored regularly and have periodic liver function tests, complete blood count, and electrolyte levels since chlorpromazine is associated with hepatotoxicity and blood dyscrasias. These laboratory assessments enable the identification of such effects at an early stage; therefore, timely action is taken to prevent further harm to the patient during the continuing treatment process.
Legal, Ethical, and Social Considerations
Prescribers should ensure that they seek consent, especially on the severe side effects and the possibility of developing tardive dyskinesia from the usage of chlorpromazine. Ethical issues involve the immediate benefits that may be accrued from the treatment against the adverse effects that may be realized in the long run, while social issues involve handling the social implications related to antipsychotic drugs. These factors are important in considering the care as a whole and patient-centered (Ricciardi et al., 2019).
Pertinent Patient Education Considerations
Patients must be advised on possible side effects of chlorpromazine, the need to follow prescription dosage, and avoid alcohol and other CNS depressants. Thus, teaching the patient about the early signs of EPS and tardive dyskinesia is crucial to prevent the worsening of the condition. Patient education ensures that patients cooperate with their treatment plan and improves therapeutic gains.
References
Gammon, D., Cheng, C., Volkovinskaia, A., Baker, G. B., & Dursun, S. M. (2021). Clozapine: Why Is It So Uniquely Effective in the Treatment of a Range of Neuropsychiatric Disorders? Biomolecules, 11(7), 1030. https://doi.org/10.3390/biom11071030
Harbell, M. W., Dumitrascu, C., Bettini, L., Yu, S., Thiele, C. M., & Koyyalamudi, V. (2021). Anaesthetic Considerations for Patients on Psychotropic Drug Therapies. Neurology International, 13(4), 640–658. https://doi.org/10.3390/neurolint13040062
Mann, S. K., & Marwaha, R. (2023, May 16). Chlorpromazine. PubMed; StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK553079/
Nucifora, F. C., Woznica, E., Lee, B. J., Cascella, N., & Sawa, A. (2019). Treatment-resistant schizophrenia: Clinical, biological, and therapeutic perspectives. Neurobiology of Disease, 131(78), 104257. https://doi.org/10.1016/j.nbd.2018.08.016
Ricciardi, L., Pringsheim, T., Barnes, T. R. E., Martino, D., Gardner, D., Remington, G., Addington, D., Morgante, F., Poole, N., Carson, A., & Edwards, M. (2019). Treatment Recommendations for Tardive Dyskinesia. Canadian Journal of Psychiatry. Revue Canadienne de Psychiatrie, 64(6), 388–399. https://doi.org/10.1177/0706743719828968
Stip, E., Rizvi, T. A., Mustafa, F., Javaid, S., Aburuz, S., Ahmed, N. N., Abdel Aziz, K., Arnone, D., Subbarayan, A., Al Mugaddam, F., & Khan, G. (2020). The Large Action of Chlorpromazine: Translational and Transdisciplinary Considerations in the Face of COVID-19. Frontiers in Pharmacology, 11(67). https://doi.org/10.3389/fphar.2020.577678
ORDER A PLAGIARISM-FREE PAPER HERE
We’ll write everything from scratch
Question
PATIENT MEDICATION GUIDE
This week, you will create a Medication Study Guide to share with your peers. This guide is intended to be a useful learning tool for you to use as you prepare for your clinical courses.
You will be assigned one of the following medications to create your guide:

Patient Medication Guide
- Chlorpromazine
- Fluphenazine
- Haloperidol
- Loxapine
- Perphenazine
- Aripiprazole
- Asenapine
- Clozapine
- Iloperidone
- Olanzapine
- Paliperidone
- Quetiapine
- Risperidone
- Ziprasidone
- Lurasidone
- Brexpiprazole
- Cariprazine
- Lumateperone
- Benztropine
- Propranolol
- Deutetrabenazine
- Valbenazine
RESOURCES
- Be sure to review the Learning Resources before completing this activity.
- Click the weekly resources link to access the resources.
WEEKLY RESOURCES
- Goldin, D. S. (2023). Fast facts for psychopharmacology for nurse practitioners. Springer Publishing.
- Chapter 7, “Antipsychotic Medications” (pp. 110–149)
- American Psychiatric Association (2020). The American Psychiatric Association practice guideline for the treatment of patients with schizophrenia. https://www.
psychiatry.org/File%20Library/ Psychiat… - Clozapine REMS (2023). What is the clozapine REMS?.https://www.
newclozapinerems.com/home# - Utah State University. (n.d.). Creating study guides.. https://www.usu.edu/
academic-support/test/ creating… - Drugs.com. (2023). https://
www.drugs.com/
TO PREPARE FOR THIS ASSIGNMENT:
- Identify your assigned psychotropic medication agent.
- Review this week’s Learning Resources, including the medication resources indicated for this week.
- Reflect on the psychopharmacologic treatments you might recommend for the assessment and treatment of vulnerable patient populations requiring antidepressant therapy.
THE ASSIGNMENT
- Create a 3- to 4-page (excluding visual elements) Medication Study Guide for your assigned psychotropic medication agents that may be utilized by you and colleagues for study. Your medication guide should be in the form of an outline and should include a title page, citations, and references. You should incorporate visual elements, such as concept maps, charts, diagrams, images, color coding, mnemonics, and/or flashcards. Be creative!
Note: Your Medication Study Guide should not be in the format of an APA paper.
Areas of importance that you should address—but are not limited to—include:
- Title page
- Description of the psychopharmacological medication agent, including brand and generic names, as well as appropriate FDA indication uses
- Any supporting, valid, and reliable research for non-FDA uses
- Drug classification
- The medication mechanism of action
- The medication pharmacokinetics
- The medication pharmacodynamics
- Appropriate dosing, administration route, and any considerations for dosing alterations
- Considerations of use and dosing in specific specialty populations, such as children, adolescents, elderly, pregnant people, those exhibiting suicidal behaviors, etc.
- Definition of half-life, why half-life is important, and the half-life for your assigned medication
- Side effects/adverse reactions potential
- Discuss clinical concerns with EPS and Tardive Dyskinesia
- Note: Be sure to include screening tools that would be utilized.
- Contraindications for use including significant drug-to-drug interactions
- Overdose considerations
- Diagnostics and labs monitoring comorbidities considerations
- Legal, ethical, and social considerations
- Pertinent patient education considerations
- References page
Support your rationale with a minimum of three (3) academic resources.
Note: While you may use the course text to support your rationale, it will not count toward the resource requirement. You should be utilizing primary and secondary literature.