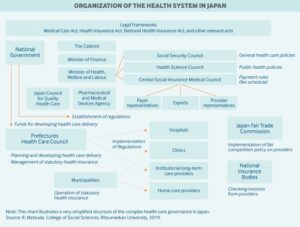
Healthcare Coverage and Quality of Japan vs USA
The statutory health insurance system in Japan provides universal coverage. The healthcare insurance system is funded primarily by individual contributions and taxes (Matsuda, 2015). Enrollment into the system is either through the residence-based or employment-based health plans and is mandatory. In addition to the monthly premiums that a person pays, a person will pay 30% of co-insurance as co-payments for a majority of the services. The co-insurance rates for low-income older persons as well as children are lower. There is also an out-of-pocket annual household maximum payment for long-term services and healthcare services that are based on income and age.
Are you interested in obtaining a unique copy on the ” Healthcare Coverage and Quality of Japan vs USA “ ? Feel free to get in touch with us.
Additionally, there are leading out-of-pocket payments that are made monthly. The national government sets the fee schedule. The prefectures in Japan develop delivery systems at the regional level (Matsuda, 2015). Most persons have private health insurance, though this is used primarily as a supplement to life insurance and provides additional income if a person becomes ill.
According to McCarthy (2015), in the U.S., healthcare is provided by several organisations comprising independent providers, hospital systems, healthcare providers, and insurance companies. Healthcare facilities are owned majorly by businesses in the private sector. In the U.S., 21% of the hospitals are in business for profit; the government owns 21%, while the majority, 58%, are community hospitals. Healthcare insurance is provided through public health coverage, such as Medicaid and Medicare, and private health insurance. Unlike most developed countries, the U.S. does not have a universal health coverage system for its people.
Japan’s healthcare insurance is employer-sponsored in the same way as that of the U.S. However, the outcomes of the two countries are vastly different. Japan is among the leading countries globally in the best-performing healthcare systems. Also, among the developed countries, Japan has the longest life expectancy. Additionally, no one in the populous nation of 130 million has ever had to file for bankruptcy because of medical bills (Matsuda, 2016)). The U.S., on the other hand, reports over 640,000 people going into bankruptcy because of medical fees. While Japan ranks at the top in the lowest rates of infant mortality (2.3 per 1,000 live births), the U.S. ranks at the very bottom with an infant mortality rate of 6.1 as of 2010 (Kim et al., 2016).
These statistics are mind-boggling, considering that Japan is the oldest country among the developed countries, with a median age of 46.9 years. This median age is ten years more than that of the U.S. If Japan were a human being, then it would be ten years older than the U.S., would live an additional six years longer than the U.S., spend 50% less in healthcare compared to the U.S., and would not be at any risk of being bankrupt (Hsu & Yamada, 2017).
Percentage of GDP Used in Healthcare in Japan and the U.S.
According to the Commonwealth Fund (n.d), Japan, in 2015, spent approximately 11% of its GDP on healthcare, of which the public financed 84% through the Statutory Health Insurance System (SHIS). 42% of the funding is from taxes, 42% from mandatory individual contributions, and 14% from out-of-pocket charges. In employment-based plans, compulsory contributions are shared between the employees and the employers. The assistance rates are approximately 10% of the monthly bonuses and the salary and are based on the employee’s income. The rates for service are capped.
The contributions are deducted from tax and vary between the prefectures and insurance fund types. For insurance plans that are residence-based, the national government funds a certain percentage of the mandatory individual contributions, as do municipalities and prefectures. Donations to the Elderly plans’ health insurance are made by the health insurance associations that insure the more prominent organizations and the Japan Health Insurance Association that certify the small and medium-sized organizations’ employers and employees. Lastly, within and among the different plans in the SHIS, there are complex cross-subsidies (Commonwealth Fund, n.d).
According to the Center for Medicare and Medicaid (CMS) (2020), the official estimates of the total spending of healthcare in the U.S. are described in the National Health Expenditure Accounts (NHEA). As far back as 1960, the NHEA has been measuring the healthcare goods and services expenditures in the U.S. every year, as well as the health insurance net cost, government administration, public health activities, and healthcare-related investment. Data presentation is by funding source, service type, and sponsor type. The healthcare expenditure in 2019 grew to $3.8 trillion, which was a 4.6% increase from the previous year and represented $11,582 per person. This amount comprised 17.7% of the GDP (CMS, 2020).
In 2019, the CMS (2020) reported that Medicare and Medicaid spending grew to $799.4 billion and $$613.5 billion and represented 6.7% and 2.9% increases, respectively, or 21% and 16%, respectively, of the total national healthcare expenditure. Private and out-of-pocket spending increased to $1,195.1 billion and $406.5 billion, 3.7% and 4.6%, respectively, for the two parameters or 31% and 11%, of the total national healthcare expenditure. Hospital expenditure also increased to $1,192.0 billion, a 2% increase from 2018 to 6.2%. Clinical services and physician expenditures increased to $772.1 billion, representing 4.6% growth from 4.0% the previous year. Lastly, 29% of the spending was federal government-sponsored, 28.4% by households, 19.1% by private businesses, 16.1% by local and state governments, and 7.5% by other personal revenues.
Japan Healthcare Achievements
The Japanese culture emphasizes eating healthy, daily mindfulness, and a healthy body. A healthy population impacts the healthcare system, while the healthcare system also makes people healthier (Borovoy & Roberto, 2015). For example, although more Japanese smoke than Americans (29.7% men and 9.7% women in Japan against the 17% average in the U.S.), the overwhelming difference lies in obesity rates in the two countries (Wise & Yashiro, 2019). The correlation between healthcare costs and obesity is well documented, with obese adults being 42% more costly and the morbidly obese being 81% more expensive compared to their leaner counterparts. In the U.S., the healthcare system spends more than $200 billion on obesity costs per annum (Wise & Yashiro, 2019). Also, there are strong relationships between being overweight or obese and osteoarthritis, atherosclerosis, strokes, cancers, diabetes, hyperlipidemia, and hypertension, all of which are costly to the healthcare system. These have a significant strain on the healthcare system in the U.S.
If the U.S. population were as lean as the Japanese populace, the outcomes on healthcare costs would be different. Japanese health is influenced heavily by their daily habits more than it is by the healthcare system. For example, the Japanese spend more time walking than the Americans do at 3.5 miles per day compared to 1 mile in the U.S. The Japanese walk more because of the high fuel costs for vehicles. Also, because the price of food in Japan is high, people are motivated to eat less, approximately 200 calories less than in the U.S. per day, with traditional foods featuring more fruits and vegetables than U.S. meals (Townsend, 2018).
The Japanese population is healthier compared to the U.S., and this makes the healthcare system less strained. Following the end of WWII, rebuilding Japan gave the country the urge to achieve universal health coverage. In 1961, a universal health coverage law was passed, and hence, close to all Japanese are covered either by the government or by their employers. Also, the fixed fee schedule means that the costs for drugs and procedures in Japan are the same everywhere (Commonwealth Fund, n.d).
Conclusion
The main flaw in the healthcare system in the U.S. is that it is employer-sponsored. However, using a similar system results in more significant outcomes in Japan. This is so because only 3.7% of the Japanese population is obese compared to 38% in the U.S.; thus, the need for healthcare is lower in the former than in the latter. Employers in Japan do not have buying leverage; therefore, insurance is less expensive for self-employed persons in Japan than in the U.S. Finally, because the Japanese population is significantly healthy, there is a minimization of healthcare system flaws such as long wait times in healthcare facilities and doctor shortages, among others.
References
Borovoy, A., & Roberto, C. A. (2015). Japanese and American public health approaches to preventing population weight gain: A role for paternalism? Social Science & Medicine, 143, 62-70.
Center for Medicare and Medicaid (2020). NHE Fact Sheet. https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/NHE-Fact-Sheet
Commonwealth Fund (n.d). International Healthcare Systems Profile: Japan. https://www.commonwealthfund.org/international-health-policy-center/countries/japan
Hsu, M., & Yamada, T. (2017). Population ageing, health care, and fiscal policy reform: the challenges for Japan. RIETI.
Kim, D. H., Jeon, J., Park, C. G., Sriram, S., & Lee, K. S. (2016). Neonatal and infant mortality in Korea, Japan, and the U.S.: effect of birth weight distribution and birth weight-specific mortality rates. Journal of Korean Medical Science, 31(9), 1450.
Matsuda, R. (2015). The Japanese health care system. International profiles of health care systems, 107-114.
Matsuda, R. (2016). Public/Private Health Care Delivery in Japan: Some Gaps in “Universal” Coverage. Global Social Welfare, 3(3), 201-212.
McCarthy, M. (2015). U.S. healthcare spending will reach 20% of GDP by 2024, says the report.
Townsend, M (2018). 3 Lessons Studying Japanese Healthcare. America Pay Attention. https://tincture.io/3-lessons-studying-japanese-healthcare-america-pay-attention-14e81a4f4002
Wise, D. A., & Yashiro, N. (Eds.). (2019). Health care issues in the United States and Japan. University of Chicago Press.
ORDER A PLAGIARISM-FREE PAPER HERE
We’ll write everything from scratch
Question
Write a 1,000- to 1,200-word essay comparing the U.S. health system to another country’s.

Healthcare Coverage and Quality of Japan vs USA
1. Describe the type of health care coverage and quality between the U.S. health system and another country.
2. What per cent of gross domestic product is used for health care, and what is the average life expectancy? Be sure to include the terms of costs, service levels, equity, access, and resource inputs for both countries.
3. Explain if the other country has achieved adequate health outcomes and if it has managed to do so for less money.
Use a minimum of three scholarly sources, including the textbook. Prepare this as an alignment according to the guidelines found in the APA Style Guide, located in the Student Success Center.
This assignment uses a rubric. Please review the title before beginning the work to become familiar with the expectations for successful completion.
You are required to submit this assignment to LopesWrite. Refer to the LopesWrite Technical Support articles for assistance.